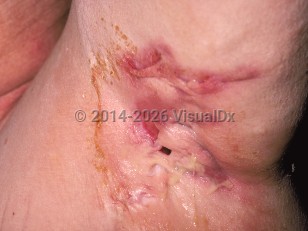
The diagnosis is clinical and based on 3 criteria:
- Typical lesions – nodules, abscesses, and tunnels (previously referred to as sinuses and fistulae)
- Recurrence – more than 2 lesions over a 6-month period
- Typical locations – primarily intertriginous
Mechanical irritation, such as by friction from tight clothing or shaving, is often reported as a trigger. The week before menses can trigger disease flares, and pregnancy and the postpartum period can be associated with either disease improvement or flaring.
Obesity and cigarette smoking are associated with HS severity but are unlikely to be the main trigger of disease in most patients. Prevalence of metabolic syndrome, major cardiovascular events, cardiac death, and diabetes (type 1 or type 2) are increased in HS compared to the general population. Regional ileitis (Crohn disease) has a statistical association with HS, while ulcerative colitis does not. People with Down syndrome are known to be at increased risk of HS. Less frequent associations are increased risk of polycystic ovary syndrome, anemia, and lymphoma.
HS is often accompanied by other disorders of the follicular occlusion tetrad, which includes acne conglobata, dissecting cellulitis, and pilonidal sinus. Associated syndromes include PASH (pyoderma gangrenosum, acne, and hidradenitis suppurativa), PAPASH (pyogenic arthritis, pyoderma gangrenosum, acne, and hidradenitis suppurativa), and PsAPASH (psoriatic arthritis, pyoderma gangrenosum, acne, and hidradenitis suppurativa), and these may, in some cases, be associated with mutations in PSTPIP1. A positive family history is reported in 30%-50% of patients in recent cohorts, and there is a 20-fold risk of disease development for those with an affected first-degree relative. Pathogenic variants affecting the gamma-secretase complex genes PSENEN, PSEN1, and NCSTN have been reported in familial cases.
There is also a strong association with mental health, including depression, anxiety, impaired sexual health, substance use disorder, and risk of suicide.
Pediatric patient considerations: HS usually presents after puberty and is more common in girls. In children presenting with early-onset disease, there is a strong association with widespread involvement, hormonal imbalance, and a strong family history. As in adults, higher rates of coexisting obesity, anxiety disorders, acne vulgaris, and acne conglobata are reported. In patients presenting who are younger than 11 years, signs of precocious puberty may be observed.



 Patient Information for
Patient Information for