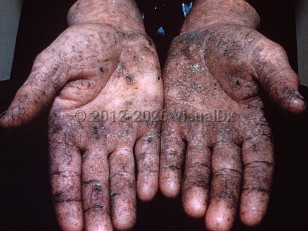
Arsenical keratosis
Alerts and Notices
Important News & Links
Synopsis

Arsenic toxicity may be acute or chronic. Mees' lines (transverse white lines seen in the nails) are a manifestation of acute toxicity. Arsenical keratoses and pigmentation represent chronic toxicity. Arsenical keratoses were first recognized in the late 1800s in the context of medicinal uses of arsenic for psoriasis, syphilis, and asthma. They are an important precursor of cutaneous squamous cell carcinoma (SCC).
Chronic arsenic poisoning is more common in male adults, but patients of any age or sex may be affected.
Pathophysiology:
The inorganic form of arsenic is more toxic than organic arsenic. Arsenic can induce chromatid exchange and cause chromosomal abnormalities in vitro; it has also been shown to modulate the expression of important transcription factors including nuclear factor kappa B, tumor suppressor p53 protein, and activating protein-1. Arsenic-related toxicity also results from the uncoupling of oxidative phosphorylation, but the exact mechanism of tumorigenesis is unknown.
Arsenic tends to concentrate in ectodermal tissues, including the skin, hair, and nails, so cutaneous manifestations are often the primary evidence of chronic toxicity.
Exposures:
Arsenical exposure often occurs accidentally, from contaminated drinking water and food and in various occupational settings. Inadvertent exposure may occur when valuable metals, such as gold and silver, are mined from arsenic ores or from the weathering of rocks containing arsenic. The arsenic fumes escape, precipitate with rain, and enter the groundwater and ultimately the drinking water. Arsenic occurs naturally in drinking water in many areas worldwide, including India, China, Taiwan, Vietnam, Laos, Cambodia, the Philippines, Bangladesh, Myanmar, Nepal, Thailand, Argentina, Chile, Mexico, Canada, and the United States. The World Health Organization (WHO)'s guideline limit is 0.01 mg arsenic per liter of drinking water. A cumulative dose of arsenic estimated to produce arsenical keratoses or cutaneous malignancies is 0.5-1 g.
Other exposures may occur in occupational settings, particularly in the agriculture industry from pesticides and herbicides. Additionally, the manufacture of computer microchips from gallium arsenide is a potential exposure risk, as are wine making, mining and smelting, carpentry, and electroplating. Toxicity can also result from intentional poisoning (suicide or crime).
Timeline:
Arsenical keratoses appear to have a latency period of approximately 20-30 years after a known exposure. SCCs (including in situ lesions) were reported to develop in pre-existing keratoses in 55% of cases in a series of Chinese patients. Metastatic SCCs have also been reported, as have basal cell carcinomas. Arsenical pigmentation may appear 6-9 years after known exposure.
Pediatric Patient Considerations:
A prior study found that in arsenic-affected districts of Bangladesh and West Bengal, 6% and 2% of the children in these respective areas compared to 24% and 11% of adults in these respective areas had arsenical skin lesions. The arsenical skin lesions that manifest in children in endemic areas are mostly diffuse or spotted melanosis, and rarely palmar or plantar keratoses. This is consistent with the long latency period for arsenical keratoses.
Chronic arsenic poisoning is more common in male adults, but patients of any age or sex may be affected.
Pathophysiology:
The inorganic form of arsenic is more toxic than organic arsenic. Arsenic can induce chromatid exchange and cause chromosomal abnormalities in vitro; it has also been shown to modulate the expression of important transcription factors including nuclear factor kappa B, tumor suppressor p53 protein, and activating protein-1. Arsenic-related toxicity also results from the uncoupling of oxidative phosphorylation, but the exact mechanism of tumorigenesis is unknown.
Arsenic tends to concentrate in ectodermal tissues, including the skin, hair, and nails, so cutaneous manifestations are often the primary evidence of chronic toxicity.
Exposures:
Arsenical exposure often occurs accidentally, from contaminated drinking water and food and in various occupational settings. Inadvertent exposure may occur when valuable metals, such as gold and silver, are mined from arsenic ores or from the weathering of rocks containing arsenic. The arsenic fumes escape, precipitate with rain, and enter the groundwater and ultimately the drinking water. Arsenic occurs naturally in drinking water in many areas worldwide, including India, China, Taiwan, Vietnam, Laos, Cambodia, the Philippines, Bangladesh, Myanmar, Nepal, Thailand, Argentina, Chile, Mexico, Canada, and the United States. The World Health Organization (WHO)'s guideline limit is 0.01 mg arsenic per liter of drinking water. A cumulative dose of arsenic estimated to produce arsenical keratoses or cutaneous malignancies is 0.5-1 g.
Other exposures may occur in occupational settings, particularly in the agriculture industry from pesticides and herbicides. Additionally, the manufacture of computer microchips from gallium arsenide is a potential exposure risk, as are wine making, mining and smelting, carpentry, and electroplating. Toxicity can also result from intentional poisoning (suicide or crime).
Timeline:
Arsenical keratoses appear to have a latency period of approximately 20-30 years after a known exposure. SCCs (including in situ lesions) were reported to develop in pre-existing keratoses in 55% of cases in a series of Chinese patients. Metastatic SCCs have also been reported, as have basal cell carcinomas. Arsenical pigmentation may appear 6-9 years after known exposure.
Pediatric Patient Considerations:
A prior study found that in arsenic-affected districts of Bangladesh and West Bengal, 6% and 2% of the children in these respective areas compared to 24% and 11% of adults in these respective areas had arsenical skin lesions. The arsenical skin lesions that manifest in children in endemic areas are mostly diffuse or spotted melanosis, and rarely palmar or plantar keratoses. This is consistent with the long latency period for arsenical keratoses.
Codes
ICD10CM:
L85.8 – Other specified epidermal thickening
SNOMEDCT:
403741004 – Arsenical keratosis
L85.8 – Other specified epidermal thickening
SNOMEDCT:
403741004 – Arsenical keratosis
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Reviewed:08/28/2017
Last Updated:09/30/2019
Last Updated:09/30/2019
Arsenical keratosis